Article Review: Prognostic value of 18F FDG and PSMA PET in patients evaluated for 177Lu Lu PSMA therapy of mCRPC
Objectives
- This study investigates the prognostic value of PSMA and [18F]FDG-PET in metastatic castration-resistant prostate cancer (mCRPC) patients considered for LuPSMA therapy.
- FDG-PET total tumor volume (FDG-VOL) was an independent predictor of overall survival (OS) in candidates for LuPSMA therapy, irrespective of subsequent treatment decision.
- PSMA-PET SUVmean was associated with biochemical response (PSA decline > 50%) to LuPSMA.
Methodology
- Retrospective analysis of 152 mCRPC patients referred for LuPSMA therapy who underwent PSMA and [18F]FDG-PET/CT.
- Visual assessment and semiquantitative measurements were performed on PET/CT images.
- Clinical and laboratory parameters were recorded.
- Overall survival (OS) and PSA response (decline > 50%) were primary and secondary endpoints, respectively.
- Statistical analysis included Kaplan-Meier analysis, Cox proportional hazards model, and logistic regression.
Results
- In LuPSMA patients, FDG-VOL was the only independent predictor of OS (HR 1.28 [95%CI 1.02-1.61]; p=0.03).
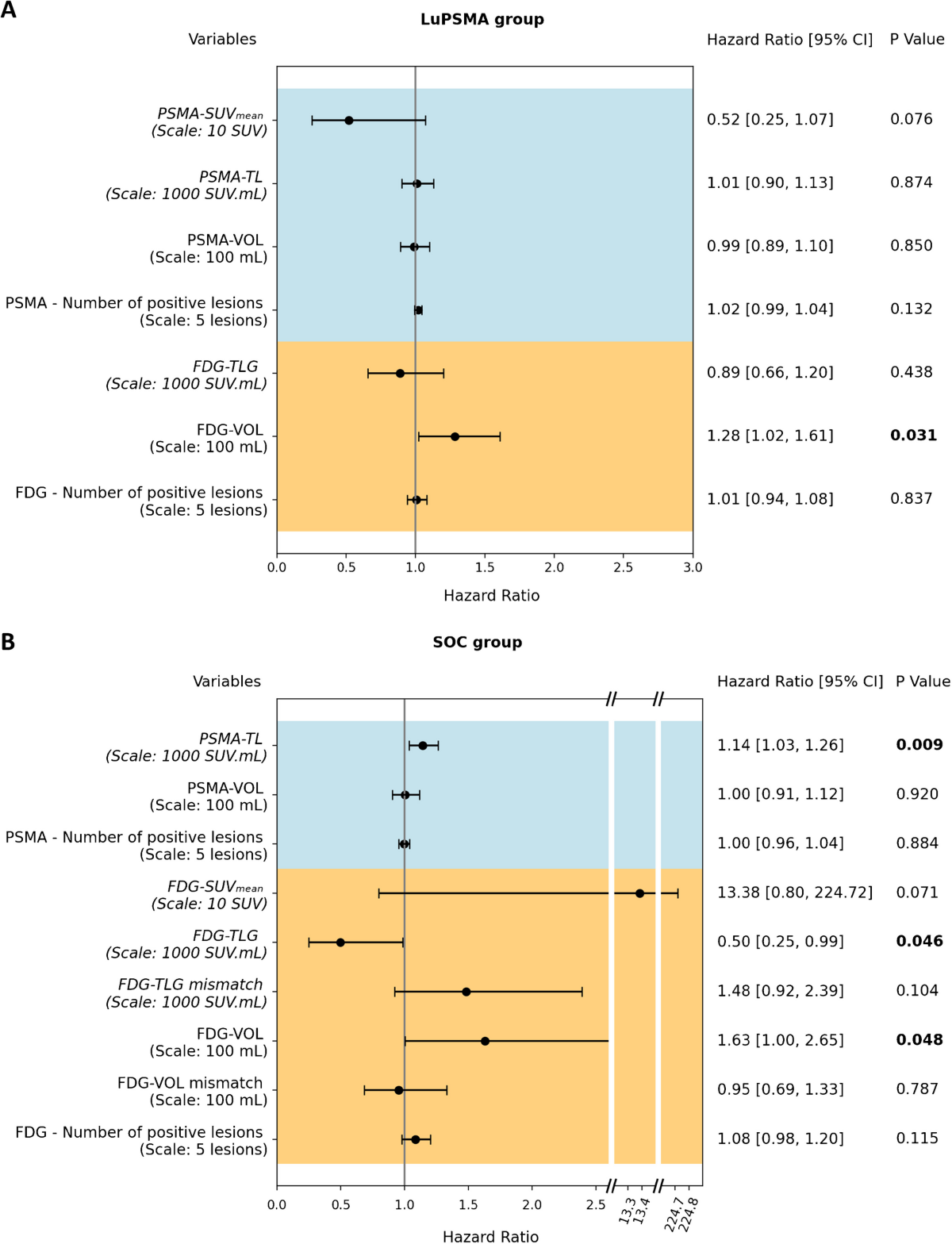
- In other SOC patients, independent predictors of OS were PSMA-TL (HR 1.14 [95%CI 1.03-1.26]; p=0.01), FDG-SUVmean (HR 20.88 [95%CI 1.2-364.74]; p=0.04), and FDG-TLG (HR 1.61 [95%CI 1.02-2.56]; p=0.04).
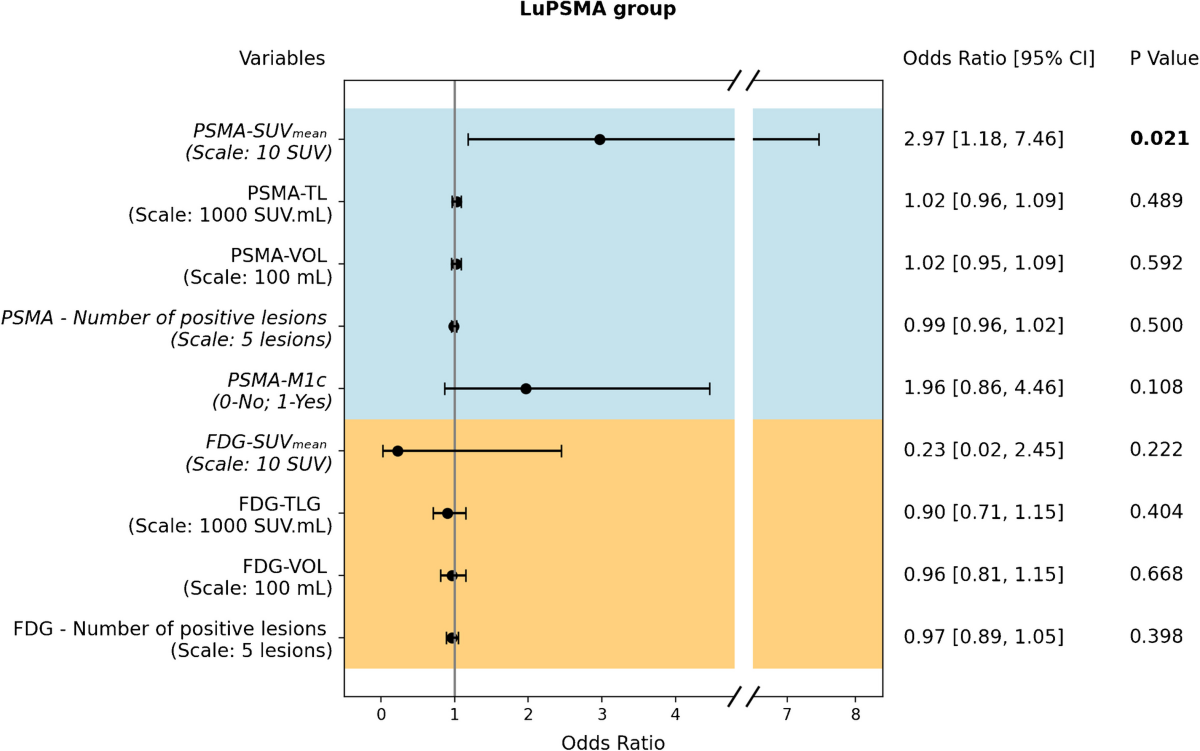
- In LuPSMA patients, PSMA-PET SUVmean was a significant independent predictor of PSA decline ≥50% (OR 2.97 [95%CI 1.27-8.16]; p=0.02).
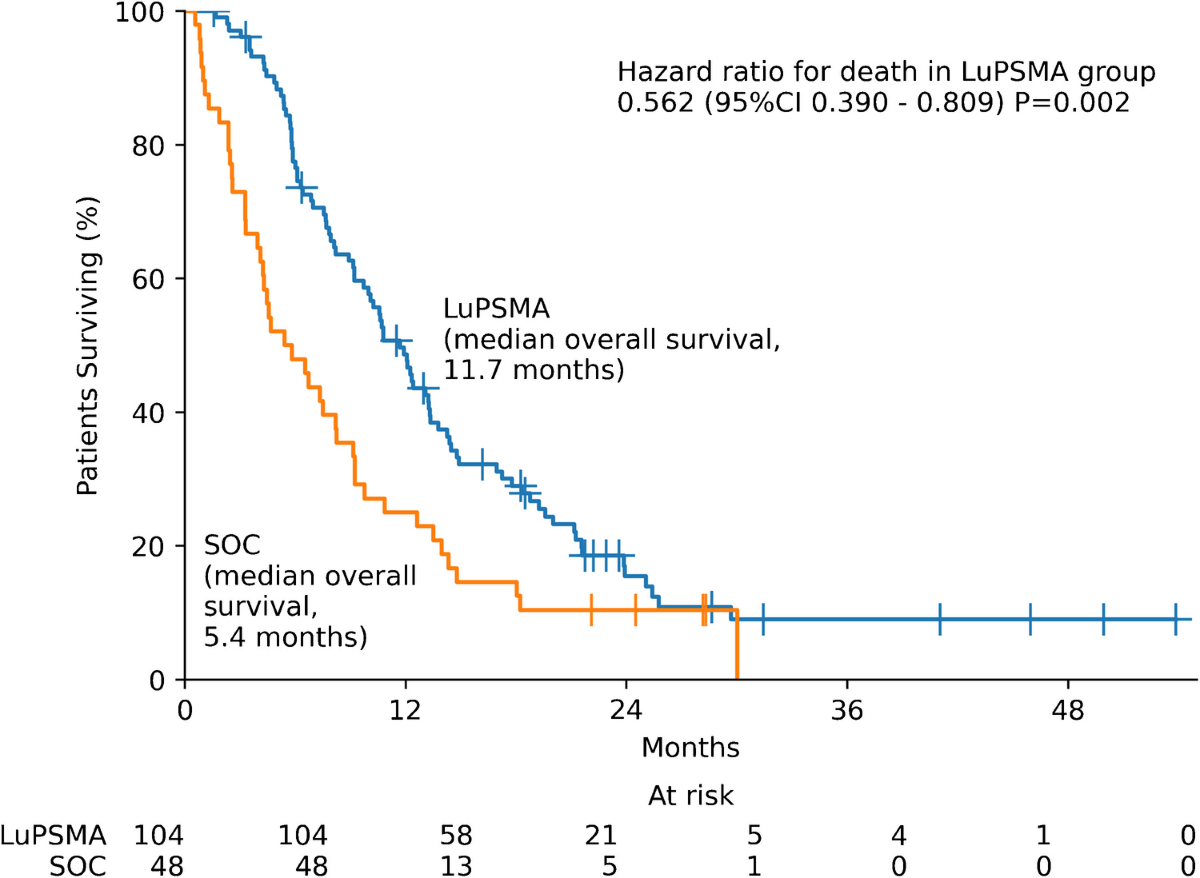
- Median OS was significantly longer in the LuPSMA group vs. the other SOC group (11.7 vs. 5.4 months, p=0.002).
- Patients with FDG-PSMA mismatch findings had a shorter OS than patients without, regardless of therapy (4.5 months vs. 10.6 months, p=0.01).
Discussions
- The study is retrospective, which introduces potential selection bias. The patient population is heterogeneous, with some patients receiving [⁶⁸Ga]Ga-PSMA-11 and others [18F]PSMA-1007, which may affect the comparability of PSMA-PET results.
- The study lacks a clear definition of "clinically significant FDG-PSMA mismatch findings," which could lead to subjective interpretation.
- The sample size for subgroup analyses (e.g., patients imaged with [18F]PSMA-1007) is relatively small, limiting the statistical power.
- The study could benefit from a more detailed description of the treatment protocols used in the SOC group.
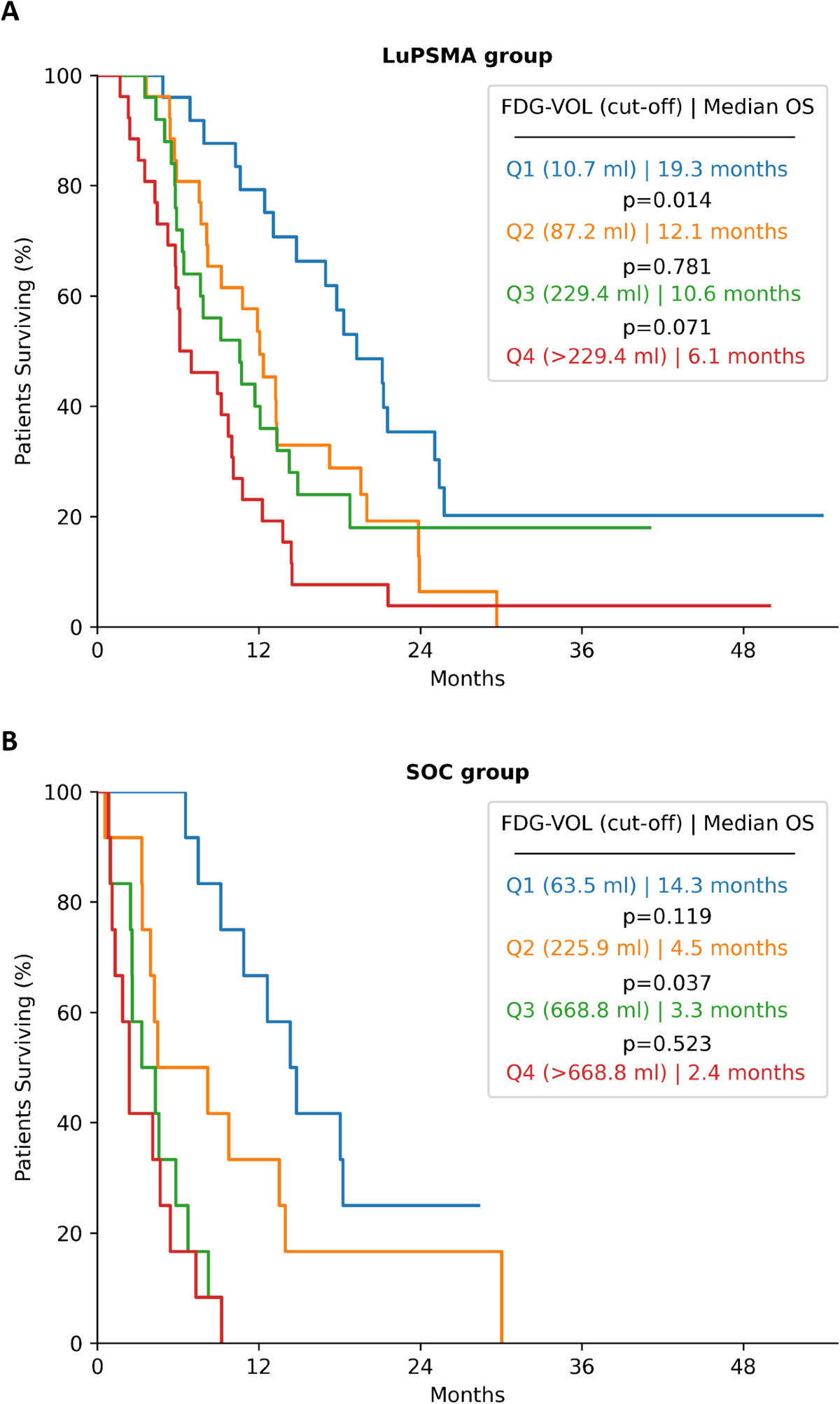
- While the study identifies FDG-VOL as an independent prognostic factor, it does not provide specific recommendations for treatment modification based on FDG-VOL.
Reference: Prognostic value of 18F FDG and PSMA PET in patients evaluated for 177Lu Lu PSMA therapy of mCRPC